 The least influential factor for caregivers was the child’s gender (Mean Rating 2.25) while appearance was seen as least important for children (Mean Rating: 2.97). Overall, the most influential factor for caregivers was the doctor’s recommendation (Mean Rating: 4.38) while the most influential factor for children was perceived to be comfort (Mean Rating: 4.20). The factors examined of potential influence on caregiver and child preferences are listed in the survey contained in Appendix 1. We hypothesized that the majority of caregivers and patients would prefer cast immobilization and that the doctor’s recommendation would strongly influence a caregiver’s immobilization preference. These topics were explored using a cross-sectional survey. The primary aim of this study was to examine caregiver and patient preferences and the factors that may influence these decisions. However, these preferences have not been formally investigated.įurther assessment of this potential implementation barrier for removable immobilization is necessary. 20 An unpublished survey of providers at our own institution indicated that persistent utilization of cast immobilization by providers was influenced chiefly by compliance concerns and the pressure of patient and caregiver preferences. 18, 19 Similar resistance to casting also exists in parts of Europe 17 despite the published guidelines supporting splinting strategies. demonstrated that patient compliance and safety are the foremost concerns impeding the use of removable splints among emergency medicine and pediatric orthopaedic physicians in North America. Prior work by this group and other investigators has sought to identify these barriers. 18, 19ĭespite the evidence supporting a new standard of care for the treatment of pediatric buckle fractures in this minimalist fashion, adoption has been slow and barriers to implementation still remain. 4– 7, 11– 15 While the minimalist approach to treatment is equally effective and decreases healthcare costs 14 and patient burden, it has not been implemented into clinical practice in all settings 16, 17 and is not the preferred method of treatment among many specialist providers. splinting) and minimal clinical and no radiographic follow-up produces the same outcome as historical treatment protocols. 3– 10 Although buckle fractures were historically managed with cast immobilization and routine radiographic monitoring, evidence emerging in the last two decades demonstrates that treatment with removable immobilization (i.e. 1, 2 Torus (buckle) fractures of the distal forearm are among the more common variants of these injuries and are characterized by an inherent stability that has enabled a recent shift towards treatment methods other than casts which were traditionally employed in the acute management of most types of pediatric forearm fractures. A torus is the convex portion of the upper part of the base of a Greek column and resembles the appearance of the cortical buckling seen in the "column" of bone which has been fractured in the pattern discussed in this article.Fractures of the distal forearm are common injuries seen in childhood and adolescence with increasing incidence. The term torus is the Latin word meaning protuberance. Sometimes a cast may be applied, but often a splint is all that is required with a period of rest and immobilization.  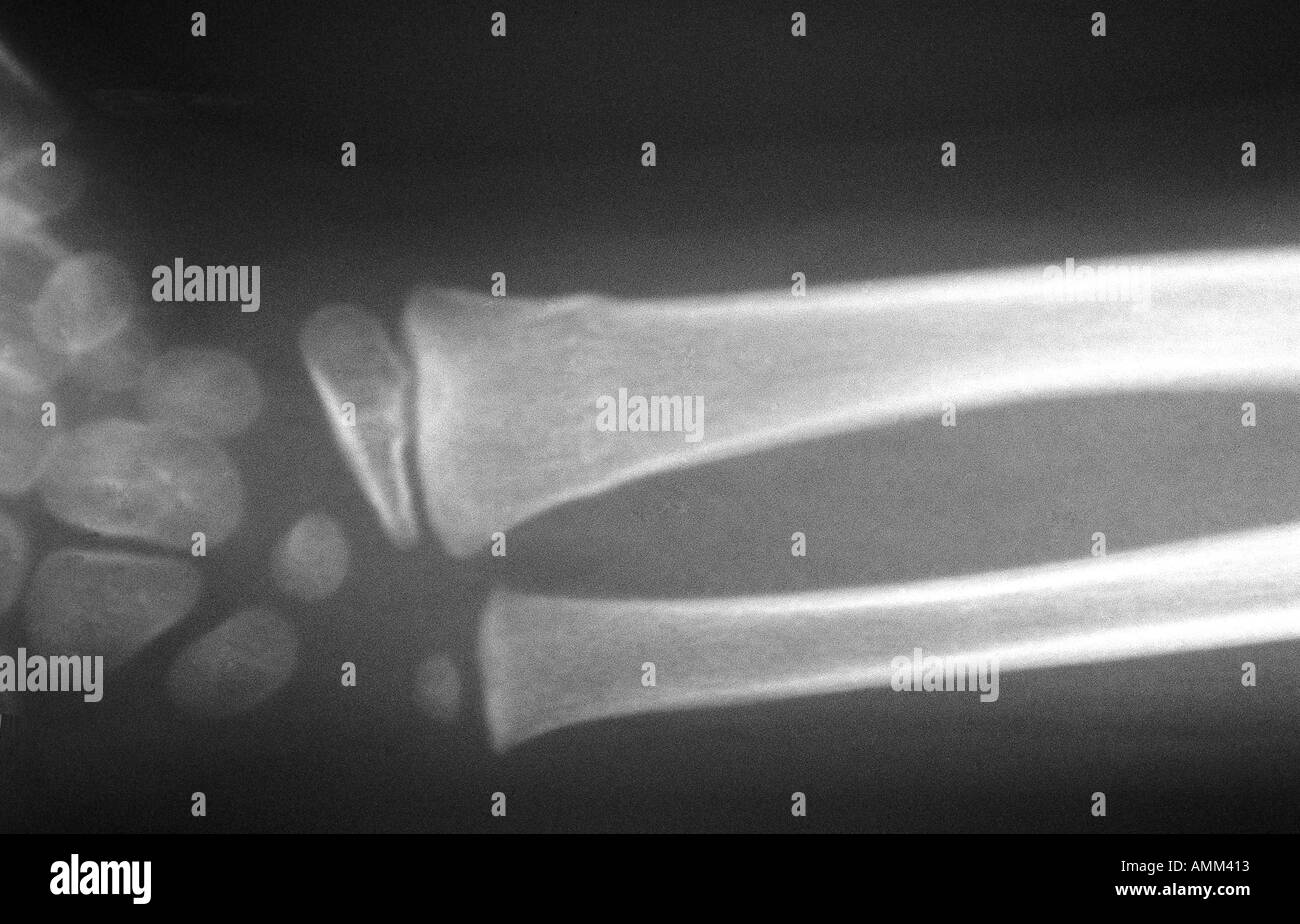
They are self-limiting and typically do not require operative intervention, although a manipulation may be required if the angulation is severe. In some cases, angulation is the only diagnostic clue Subtle deformity or buckle of the cortex may be evident This most commonly occurs at the distal radius or tibia following a fall on an outstretched arm the force is transmitted from carpus to the distal radius and the point of least resistance fractures, usually the dorsal cortex of the distal radius. Cortical buckle fractures occur when there is axial loading of a long bone. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
